Endometriosis
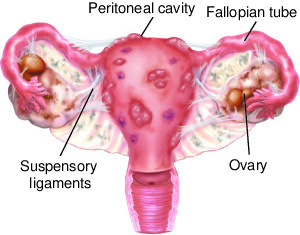 Endometriosis (en-doe-me-tree-O-sis) is an often painful disorder in which tissue similar to the tissue that normally lines the inside of your uterus — the endometrium — grows outside your uterus. Endometriosis most commonly involves your ovaries, fallopian tubes and the tissue lining your pelvis. Rarely, endometrial-like tissue may be found beyond the area where pelvic organs are located.
With endometriosis, the endometrial-like tissue acts as endometrial tissue would — it thickens, breaks down and bleeds with each menstrual cycle. But because this tissue has no way to exit your body, it becomes trapped. When endometriosis involves the ovaries, cysts called endometriomas may form.
Surrounding tissue can become irritated, eventually developing scar tissue and adhesions — bands of fibrous tissue that can cause pelvic tissues and organs to stick to each other. Endometriosis can cause pain — sometimes severe — especially during menstrual periods. Fertility problems also may develop. Fortunately, effective treatments are available.
Endometriosis (en-doe-me-tree-O-sis) is an often painful disorder in which tissue similar to the tissue that normally lines the inside of your uterus — the endometrium — grows outside your uterus. Endometriosis most commonly involves your ovaries, fallopian tubes and the tissue lining your pelvis. Rarely, endometrial-like tissue may be found beyond the area where pelvic organs are located.
With endometriosis, the endometrial-like tissue acts as endometrial tissue would — it thickens, breaks down and bleeds with each menstrual cycle. But because this tissue has no way to exit your body, it becomes trapped. When endometriosis involves the ovaries, cysts called endometriomas may form.
Surrounding tissue can become irritated, eventually developing scar tissue and adhesions — bands of fibrous tissue that can cause pelvic tissues and organs to stick to each other. Endometriosis can cause pain — sometimes severe — especially during menstrual periods. Fertility problems also may develop. Fortunately, effective treatments are available. - Superficial peritoneal lesion : This is the most common kind. You have lesions on your peritoneum, a thin film that lines your pelvic cavity.
- Endometrioma (ovarian lesion) : These dark, fluid-filled cysts, also called chocolate cysts, form deep in your ovaries. They don’t respond well to treatment and can damage healthy tissue.
- Deeply infiltrating endometriosis : This type grows under your peritoneum and can involve organs near your uterus, such as your bowels or bladder. About 1% to 5% of women with endometriosis have it.
- Retrograde menstruation : In retrograde menstruation, menstrual blood containing endometrial cells flows back through the fallopian tubes and into the pelvic cavity instead of out of the body. These endometrial cells stick to the pelvic walls and surfaces of pelvic organs, where they grow and continue to thicken and bleed over the course of each menstrual cycle.
- Transformation of peritoneal cells : In what’s known as the “induction theory,” experts propose that hormones or immune factors promote transformation of peritoneal cells — cells that line the inner side of your abdomen — into endometrial-like cells.
- Embryonic cell transformation : Hormones such as estrogen may transform embryonic cells — cells in the earliest stages of development — into endometrial-like cell implants during puberty.
- Surgical scar implantation : After a surgery, such as a hysterectomy or C-section, endometrial cells may attach to a surgical incision.
- Endometrial cell transport: The blood vessels or tissue fluid (lymphatic) system may transport endometrial cells to other parts of the body.
- Immune system disorder: A problem with the immune system may make the body unable to recognize and destroy endometrial-like tissue that’s growing outside the uterus.
- Back pain during your period
- Severe menstrual cramps
- Pain when pooping or peeing, especially during your period
- Unusual or heavy bleeding during periods
- Blood in your stool or urine
- Diarrhea or constipation
- Painful sex
- Fatigue that won’t go away
- Trouble getting pregnant
